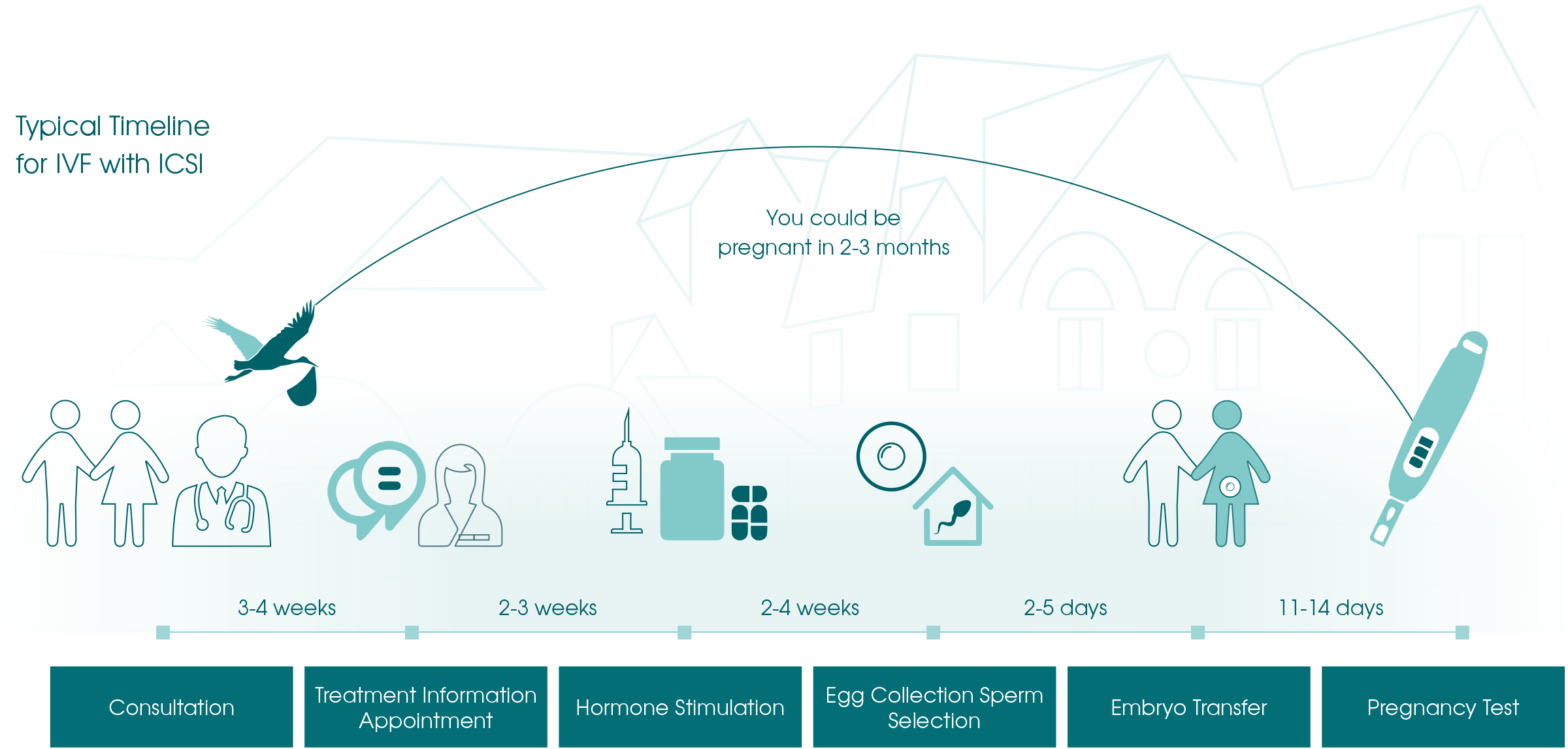
In-Vitro Fertilisation (IVF)
IVF is a type of fertility treatment where the eggs are removed from the ovaries and fertilised by sperm in a dish in the laboratory.
What is IVF?
In Vitro Fertilisation (IVF) means “fertilisation in glass”, and is so named as eggs are removed from the ovaries and fertilised by sperm in a dish in the laboratory.
The resulting embryos are cultured for 3-5 days, after which the best embryo/embryos are transferred into the uterus or stored for future use, a standard fertility procedure at the Herts & Essex Fertility Centre.
Who is it for?
The indications for recommending IVF treatment are as follows:
- Blocked or damaged fallopian tubes
- Unexplained infertility
- Following unsuccessful treatment with IUI or Ovulation Induction
- Polycystic Ovarian Syndrome
- Endometriosis
When is IVF recommended?
IVF is only appropriate if the parameters of the sperm sample provided on the day of egg collection are within normal ranges.
The sperm sample is prepared by a washing technique in the laboratory, and a known concentration of the prepared sperm sample is added to a culture dish containing your collected eggs. The inseminated eggs are incubated overnight which gives the sperm an opportunity to fertilise the mature eggs. The following morning the inseminated eggs are assessed for signs of fertilisation by one of our embryologists. On average 60-70% of eggs will fertilise if the sperm sample is suitable for IVF treatment.
IVF with a sperm sample that is not within normal ranges can significantly reduce the likelihood of fertilisation. If your sperm sample on the day of egg collection is no longer within the normal ranges, we can easily convert your treatment cycle from IVF to ICSI. We will help you make a fully informed decision by discussing your treatment and answering any questions you may have before proceeding.
Step 1
Suppressing the natural monthly cycle (downregulation)
Downregulation is by medication to make your ovaries temporarily inactive, for easier management of your treatment cycle during stimulation with daily hormone injections. This protocol is used in women with normal ovarian reserve. There is a different protocol for women with poor ovarian reserve.
Step 2
Boosting your egg supply
Once your natural cycle is suppressed, you will have daily Follicle Stimulating Hormone (FSH) injections to promote the development of multiple follicles in your ovaries. FSH will increase the number of eggs you produce, allowing us to create more embryos and thus give greater choice for use in your treatment.
Step 3
Egg retrieval
During egg collection you will be in deep sedation, calm, relaxed and unlikely to feel any pain. Under sedation, our Fertility Consultant will extract your eggs using a special needle introduced vaginally under ultrasound guidance. Each follicle is aspirated individually until all visible follicles are drained from both ovaries. The procedure will take approximately thirty minutes, after which you will return to the recovery room to be cared for by our specialist nursing team.
Step 4
Collecting sperm
Following admission, the male partner will provide a fresh semen sample to be checked for quality and prepared by a special washing technique in the laboratory. A known concentration of the prepared sperm sample is added to your collected eggs in a culture dish and incubated. If you are using donated sperm, your selected donor sperm is removed from frozen storage, thawed and prepared in the same way.
Step 5
Fertilisation of eggs in the laboratory
Your eggs are mixed with the sperm and incubated overnight to allow fertilisation to take place. The embryologist will assess the inseminated eggs for signs of fertilisation the following morning. On average, 60–70% of eggs will fertilise normally with the sperm provided at egg collection. Depending on the number of eggs that have been fertilised, your transfer will be scheduled for either Day 3 or Day 5 of culture.
If your sperm sample on the day of egg collection is not within normal range, we can easily convert your IVF treatment cycle to ICSI whereby a single normal sperm is selected and injected directly into each egg.
Step 6
Embryo transfer
Embryo transfers can take place on day 3 day 5. If there are still embryos in culture after embryo transfer, or if a transfer is not planned for your cycle, then embryos are assessed on days 5 and 6 for their suitability to be frozen for future use. If they are good-quality blastocysts and contain the visible and necessary structures known to give rise to a pregnancy, they can be frozen for use in the future.
We strongly believe that embryos should be replaced at the optimum stage of development, after proving themselves by a process of self-selection. It is for this reason that Herts & Essex perform embryo transfer seven days a week, on Days 3 and 5 following collection.
For women under the age of 40, one or two embryos can be transferred. If you are over 40, a maximum of three embryos can be returned. The number of embryos transferred is restricted because of the risks associated with multiple births. If the remaining embryos are suitable they may be frozen for future use.
![]()