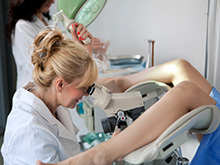
Gynaecology scan
A gynaecology scan is an ultrasound scan procedure to examine your pelvic organs (ovaries, fallopian tubes, and uterus). The scan is performed by one of our experienced Consultant Gynaecologists, who will begin by asking you about your symptoms.
Our state of the art medical facilities offers prompt diagnosis and management of simple as well as complex gynaecological conditions in a calm and relaxing environment. Advanced ultrasound technology including 3D and 4D contrast sonography optimises our accuracy.
Our team of experienced consultant gynaecologists will perform the tests, discuss the results, and offer a management plan most suitable for you.
Show more
Where surgical intervention is required, the latest minimally invasive techniques are used, with a very short hospital stay and recovery period.
The scan provides detailed images to confirm that the pelvic organs are normal or the presence of abnormalities such as:
- Fibroids
- Endometrial polyps
- Ovarian cysts
- Endometriosis
- Polycystic ovaries
- Premature ovarian insufficiency (also known as premature menopause)
- Ovarian cancer screening
Ultrasound services offered at Herts & Essex Fertility Centre:
- 2D and 3D ultrasound of ovaries and uterus (womb)
- 3D saline infusion sonography of the womb cavity (where indicated)
When should you have a gynaecology scan?
Gynaecology scans are recommended if you suspect, or have experienced, one of the following symptoms:
- Irregular or heavy periods
- Bleeding after menopause
- Fibroids
- Pelvic pain
- Difficulties conceiving
What happens during a gynaecology scan?
In most cases, an ultrasound scan via the transvaginal route is normally performed. This is an internal investigation and performed with an empty bladder. However, if an internal ultrasound scan is inappropriate or not possible, an abdominal ultrasound scan will be performed, although the views and detail are occasionally not as good as those from an internal scan.
Gynaecology scans should not be uncomfortable and are usually completed in half an hour. Once the scan is finished our consultant will discuss the results and provide the most suitable management plan for you.
How much is a gynaecology scan?
The consultant gynaecologist will talk you through the procedure and inform you of the findings as it is performed.
Do I need a GP or hospital referral?
When possible we offer both same-day and next-day appointments for your gynaecology scan and you do not need a GP or hospital referral. Our consultant gynaecologist will provide you with a complimentary printed report that you can take to your GP to discuss the results, should you wish to.
Show less
![]()
Polycystic Ovary Syndrome (PCOS)
Polycystic ovary syndrome (PCOS) is a common hormonal problem that affects 5-10% of all women of child-bearing age. It is the most common female hormonal problem and one that can have significant bearing on female fertility, although it is worth knowing that having polycystic ovary syndrome does not necessarily make you infertile, and many women with PCOS get pregnant.
The common signs and symptoms of PCOS include irregular or absent periods, excess body fat, excess facial hair, oily skin or acne, difficulty maintaining weight and difficulties getting pregnant. Women with PCOS are predisposed to developing Type 2 diabetes, heart disease and endometrial cancer (cancer of the womb lining) later in life.
Show more
Where PCOS features in female infertility, the usual problems are irregular ovulation or anovolution (this is when the ovaries fail to release egg cells during the menstrual cycle. We have found that management of this common condition is often disjointed, with many women unsure about the diagnosis or management options.
You can be reassured that our comprehensive and integrated service is provided by our team of highly experienced reproductive medicine consultants, gynaecology nurses and counsellors. We investigate the cause of your PCOS thoroughly, identify the most appropriate means of treatment – for all aspects of the condition, including infertility, menstrual irregularity, skin problems and weight concerns – and we provide complete follow-up and support throughout the process. In the majority of cases where irregular ovulation or anovulation is responsible for your infertility, we can successfully treat you. Where amenorrhoea (the complete absence of a menstrual period) is encountered, successful treatment is also possible. In those cases where amenorrhoea cannot be corrected, we offer full counselling and can advise you on alternative routes to pregnancy, such as IVF or ICSI.
Show less
![]()
Premature ovarian ageing
As women age their reserve of eggs available for monthly ovulation naturally declines. However, one in ten women experience a significant decline in egg reserve earlier than they should, and this is known as premature ovarian ageing (POA). If you suffer from an autoimmune disorder (eg thyroid disease or rheumatoid arthritis), endometriosis or have had any operations involving your ovaries, you are particularly at risk of premature ovarian ageing (POA).
Women with POA typically have difficulty conceiving naturally, or even with the help of fertility treatment, especially if that treatment is not right for their fertility status. A prompt diagnosis and early treatment are vital because the decline in ovarian reserve can be quite rapid once it begins.
Show more
A simple blood test for Anti-Mullerian Hormone – AMH and follicle stimulating hormone – FSH together with an ultrasound scan (antral follicle count) with age-specific interpretation will diagnose the condition.
While premature ovarian failure (POF) for the most part requires donor eggs for a successful pregnancy, we have above-average success rates in treating carefully selected patients with premature ovarian ageing using their own eggs.
| Treatment | Cost(£) | |
|---|---|---|
| Female Fertility Assessment:
1st visit AMH (Anti-Mullerian hormone) – to assess the patient’s ovarian reserve Thyroid function test (TFT) [Thyroxine T4 & Thyroid stimulating hormone (TSH)] 2nd visit Ultrasound scan with antral follicle count Consultation during a scan appointment |
£450 |
Show less
![]()
Premature ovarian failure
Premature ovarian failure (POF) is another term for the early onset of female menopause. When a woman’s ovaries stop producing oestrogen, menopause will begin. The average age at the onset of menopause is 51, but early menopause can occur before 40 years of age. Unfortunately, about 10% of all women are affected by premature ovarian failure. It is a very dramatic-sounding term, but it does not mean we cannot help you to become pregnant.
There are lots of reasons why women have premature ovarian failure. Various genetic factors, autoimmune disorders, surgical removal of ovaries and receiving cancer treatments are among the most common causes. As menopause occurs your eggs will no longer be viable. Unfortunately, there are no treatments available to produce new eggs, therefore, fertility treatment with donor eggs is usually the only option for women with premature ovarian failure.
Hormone replacement therapy (HRT)
As well as infertility, ovarian failure can create other problems for women. These too can be overcome provided they are identified and treated appropriately. The ovaries are responsible for producing oestrogen, the main female sex hormone. Among many other functions, oestrogen plays an important role in maintaining bone strength, decaying teeth and hair loss, and preventing vaginal dryness. Low oestrogen production can leave bones susceptible to fractures. Hormone replacement therapy (HRT) may be appropriate in some cases. In addition to this, close monitoring of bone strength using a bone density scan can greatly reduce any risk of bone damage.
If you are concerned about irregular menstrual cycles or think that you may be at risk of early menopause or premature ovarian failure, and you would like to discuss the possible implications for your fertility, call us on 01992 78 50 60 to book a confidential appointment.
Recurrent miscarriage
Miscarriage is the spontaneous loss of a pregnancy before 24 weeks gestation. Miscarriages, and recurrent miscarriage, are highly traumatic, frustrating experiences that leave women and their partners despairing of their chances of having a baby.
Recurrent miscarriage is defined as three consecutive miscarriages. Sporadic pregnancy loss is a non-recurring miscarriage. Most sporadic pregnancy losses can be attributed to foetal chromosome abnormalities that occur at random. Fewer than 5% of women have two consecutive miscarriages and only 1%-2% suffer three or more miscarriages consecutively.
It is not always possible to identify and treat recurrent pregnancy loss. Sometimes the cause of recurrent miscarriage is identifiable and treatable, leading to successful future pregnancies. Unfortunately, in most cases either a diagnosis cannot be reached or treatment is not possible.
We run a comprehensive pregnancy loss service, looking after women who have experienced miscarriages with or without fertility treatment. You will have a consultation with a specialist and based on your history and investigations, treatments may be available to achieve a successful pregnancy.
Investigation packages to identify the cause of recurrent miscarriage include:
| Treatment | Cost* | |
|---|---|---|
| Miscarriage Testing | Cost (£) | |
| Recurrent miscarriage profile (3D ultrasound scan, Thrombophilia screen, Antiphospholipid screen, Thyroid screen, Female Karyotype, follow up discussion with a consultant regarding results) | £1,820 | |
| Extended recurrent miscarriage profile (3D ultrasound scan, Thrombophilia screen, Antiphospholipid screen, Thyroid screen, Male & Female Karyotype, follow up discussion with a consultant regarding results) | £2,340 |
![]()
Gynaecological surgery
As part of your pre-treatment assessment at the Herts & Essex Fertility Centre, we will check for common gynaecological conditions such as uterine fibroids, polyps, ovarian cysts and blocked and dilated fallopian tubes (hydrosalpinx). Some of these conditions can be readily resolved and could restore your natural fertility and ability to conceive. Where fertility treatment is needed, we carry out surgery to maximise your chances of a successful pregnancy.
Show more
Your peace of mind matters, so it is reassuring to know that as one of the best IVF clinics in the UK, our gynaecological surgery team has decades of experience. Surgery is only ever undertaken where it is to your advantage and of minimal risk. The surgery is discussed with you in detail and performed by our own reproductive surgery specialists. Where a referral to other specialists is necessary, detailed information is provided, including recommendations, thus maximising surgical benefit.
Typical gynaecology surgery at the Herts & Essex Fertility Centre includes:
Laparoscopic surgery
This is keyhole surgery – a technique involving only small incisions – for assessing the pelvis, removing scar tissue (also known as adhesions), managing ovarian cysts and treating hydrosalpinx and ectopic pregnancies.
Hysteroscopic surgery
A camera is inserted into the womb through the cervix. To confirm the presence of uterine fibroids, polyps, and scar tissue surgically treated.
Open surgery
For large fibroids, open surgery may be required.
Surgical management of miscarriage
Miscarriage following fertility treatment or natural conception is very traumatic. You will be offered management choices, either wait for natural resolution or proceed with surgical treatment. This is available at Herts & Essex Fertility Centre, providing convenient management with your familiar clinical team at a very stressful time.
Vacuum or suction aspiration is used to remove uterine contents through the cervix. It may be used as a method of induced abortion, a therapeutic procedure used after miscarriage, or as a procedure to obtain a sample for endometrial biopsy.
| Treatment | Cost(£) | |
|---|---|---|
| MVA with histology | £950 | |
| Karyotyping MVA | £385 |
Show less






